Introduction
Functional Capacity Evaluations (FCEs) help determine a person's ability to complete work-related tasks safely after an injury or illness. In physical and occupational therapy, an FCE is most valuable when it is consistent, clinically grounded, and clearly documented. That is where the Kinesiophysical Method stands out.
The Kinesiophysical Method combines anatomy, biomechanics, and careful observation to evaluate performance and effort during progressively demanding tasks. It supports defensible conclusions while keeping patient safety at the center of every decision.
The therapist's role in an FCE
Physical and occupational therapists are uniquely qualified to complete FCEs because our training integrates movement science, pathology, and functional performance. That foundation supports accurate task selection, appropriate progression, and meaningful interpretation of what we observe.
An effective FCE does more than list limitations. It identifies safe functional abilities, clarifies barriers to work performance, and informs next steps for rehabilitation or job planning. The goal is practical: help the individual move toward safe, sustainable function at work and in daily life.
What the Kinesiophysical Method is
The term kinesiophysical connects two essentials: movement and the body's physiological and biomechanical responses. In practice, it is a structured way to interpret how the body performs under physical demand, especially as fatigue and symptoms change task quality.
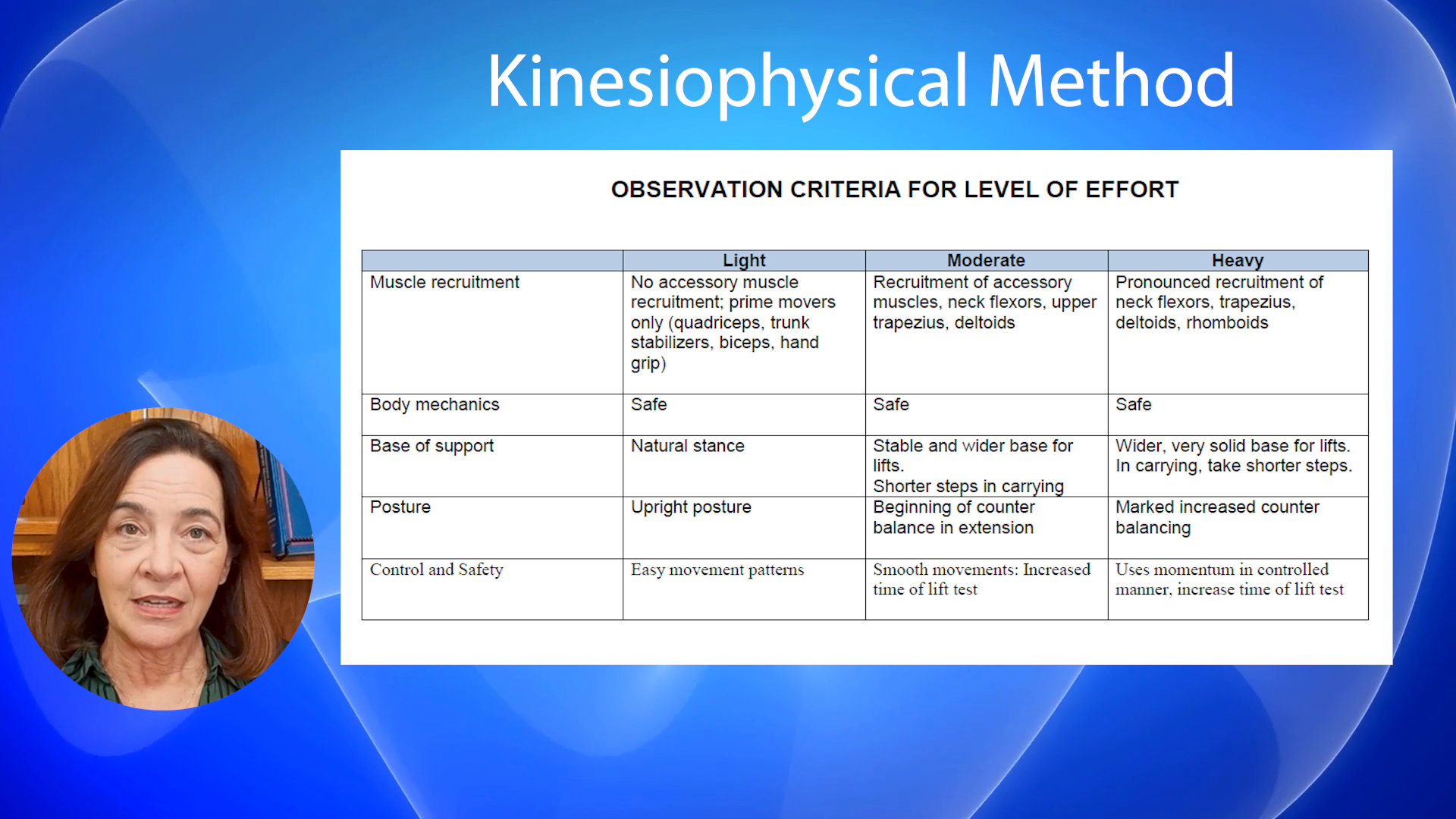
Rather than relying on a single measure, the method uses observation standards to judge control, movement patterns, and physiological response. This helps the therapist identify when performance is safe and when it becomes inefficient, risky, or inconsistent with the stated capacity.
How the process works in practice
An FCE using the Kinesiophysical Method begins with a careful review of medical records. History matters because prior injuries, surgeries, and chronic conditions influence safe task selection and expectations for performance.
Next comes a physical examination to establish a baseline of strength, mobility, and symptom behavior. The evaluation then progresses through test items that simulate job tasks. Demands increase in a controlled way while the therapist monitors movement quality, symptom response, and signs that indicate the task should be modified or stopped.
Case example: chronic knee condition
Consider a patient returning to work with a chronic knee condition. Early in testing, walking may look safe and stable with no obvious impairments. That initial observation alone can be misleading if it is not followed by progressive functional demands.
As tasks become more challenging, subtle signs can appear. During a floor-to-waist lift, the descent may become less controlled or the patient may guard the knee. Stair climbing may reveal reduced ability to control body weight, especially when fatigue builds.
Using kinesiophysical observation criteria, the therapist notes effort level and whether movement remains controlled. When control decreases, compensation increases, or symptoms escalate, those are clinically meaningful findings and often the point where safety dictates stopping or adjusting the activity.
Safety, ethics, and therapist-patient communication
Safety is the non-negotiable standard in every FCE. Patients have the right to decline any part of testing, and the therapist has the responsibility to stop tasks when signs of unsafe performance emerge. Ethical practice also means reporting what is observed clearly and without bias so recommendations support safe work environments.
Therapist-patient interaction directly affects the quality of the evaluation. Clear instructions, supportive communication, and a calm pace help the patient understand expectations and perform consistently. This creates better data for decision-making and a more respectful experience for the person being evaluated.
Learn and grow
If you want to build stronger clinical confidence in functional capacity evaluation, explore our resources and training on our Functional Capacity Evaluation page. A structured approach to observation, progression, and documentation helps you produce safer evaluations and more defensible reports.